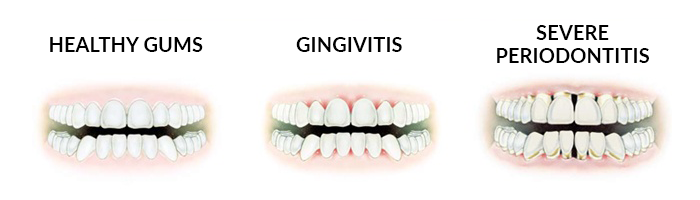
Periodontitis
Sonria Dental is a periodontal surgery London and gum disease specialist Central London. A healthy mouth is colonised by 200 to 300 bacterial species. Most of this bacteria are completely harmless and live in harmony in your mouth. However, when tooth cleaning is not thorough enough, the bacterial deposits build up next to the gums, forming a plaque. The conditions, therefore, gradually, become suitable for more dangerous bacteria to flourish, ultimately, compromising the body’s defences.
What is Periodontitis?
Periodontitis, often known as ‘gum disease’, is one of the most common human diseases. Gum disease is a very common condition in which the gums and deeper periodontal supporting structures become inflamed. This inflammation of the gums, which usually takes the form of redness, swelling and a tendency to bleed during tooth brushing, is the body’s response to periodontal bacteria that have been allowed to accumulate on the teeth.
The inflammation of the gums and supporting structures is the body’s defence system. However, this inflammatory response can eventually cause serious damage. If left unchecked, the inflammation can spread down below the gums and along the roots of the teeth, causing destruction of the periodontal ligament and the supporting bone. This ultimately leads to the loosening and potential loss of the teeth.
How does periodontal bacteria build up?
Although periodontal bacteria is naturally present in the mouth, they are only harmful when the conditions are right for them to increase in numbers. This bacteria, however, will build up in numbers when layers of bacteria and food debris, known as plaque, is left undisturbed on the teeth, commonly in hard-to-reach areas such as between the teeth. Here, the more dangerous bacteria are able to thrive, producing harmful by-products that cause inflammation of the gums. This inflammation is referred to as gingivitis.
Symptoms of Periodontitis:
- Periodontitis begins with gingivitis (inflammation of the gums);
- Gums that feel tender when touched;
- Bleeding from the gums when you brush your teeth, eat, or even spontaneously;
- Painful chewing;
- Discoloured layer of bacterial plaque on the teeth;
- Bad breath;
- Changes in the positioning of the teeth;
- Pus between your teeth and gums;
- Gum recession; and
- Pain in the mouth, teeth, and/or jaw.
Please note – bleeding from the gums may be less noticeable in smokers!
What happens if bacterial plaque is not removed?
As a gum disease specialist Central London we are of the view that if the bacterial plaque is not removed from the gums and surfaces of your teeth while it is still soft, overtime, minerals are deposited and it can become a harder substance called tartar.
The more tartar is present, and for longer periods of time, the growth of bacterial plaque towards the root of the tooth is encouraged, This, then, causes an inflammatory reaction deeper into the gums, causing a disruption in the attachment of the gum to the root, causing a gap, known as periodontal pocket. This pocket then become an ideal habitat for further harmful bacteria to colonise and multiply, therefore driving the disease process forward. As the bacteria continues to invade, they release toxins as products of their metabolism, which further trigger the body’s defence mechanisms.
If periodontal inflammation is not treated, the supporting structures of the teeth, including the surrounding bone, can be destroy. Therefore, with no supporting structure, teeth can become loose overtime, and eventually fall out. If not lost, you may require an extraction of the affected teeth, as well as the above described symptoms.
Factors that increase the severity and speed of progression of periodontitis:
Treating periodontal disease:
The key to success is to eliminate the bacterial plaque that triggers the periodontal disease process and to establish excellent oral hygiene practices. However, when a patient is suffering from periodontitis, there are a few options for treatment:
Read our in house article, from the point of view of a gum disease specialist Central London on How to treat bleeding gums / gingivitis.
We can also advise on periodontal scaling and root planing cost, periodontist cost from the pov of a London periodontist. There is no such thing as an average cost of periodontal treatment. We are a periodontist Harley Street and would be happy to discuss with and advise you on periodontal disease treatment options.
We do have gum surgery before and after photos which we are happy to show you.
For more information regarding the topic of periodontitis, please visit the following websites:
Corsodyl
The British Society of Periodontology
European Federation of Periodontology